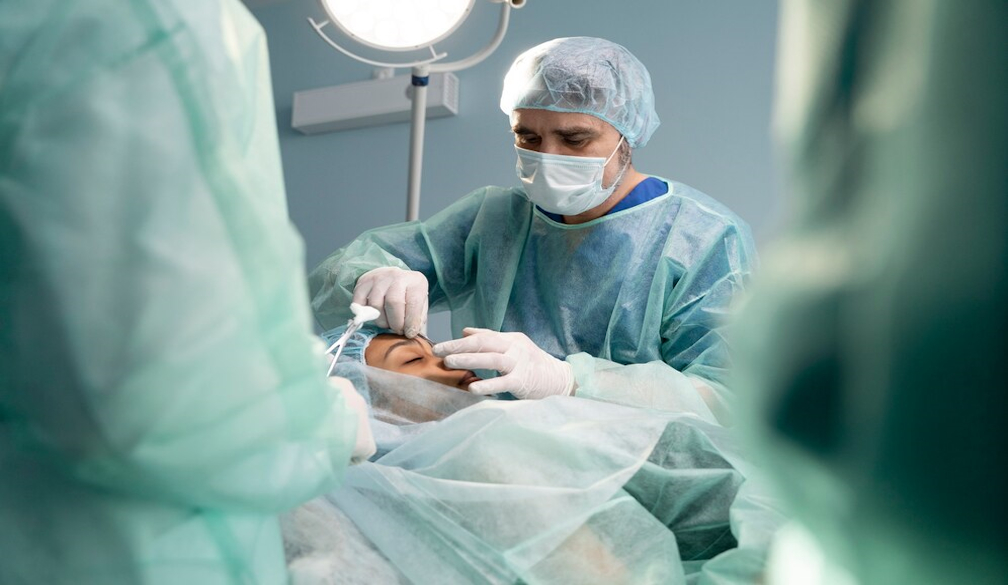
Primary care involves more than GPs. A new review shows how patients can better access care

Australians today are more likely than previous generations to live with complex and chronic diseases, such as diabetes, heart disease and depression.
This means they’re more likely to need health care from a variety of different providers, such as nurses, podiatrists, psychologists and physiotherapists, as well as GPs. This is known as “multidisciplinary care”. It works best when the skills of all these professions are available to the patient in a co-ordinated way.
But the roles of health professions, and the way they’re funded, have been frozen in legislation and policy for decades. Any change has been incremental and disjointed. It has mostly involved adding more items to the Medicare schedule, with each professional practising separately.
The result has been greater inequity of access. Because fewer than half of allied health fee-for-service visits are bulk-billed, most patients pay almost A$70 for each consultation – and sometimes much more. Those who can’t afford the out-of-pocket costs and can’t find a bulk-billing practitioner miss out.
To assess how the government can remove barriers to team-based care and get health professions working to their full potential, or their full “scope of practice”, last year the government commissioned an independent review.
The final report, released yesterday, sets a new path for the primary care workforce. This could make multidisciplinary care within reach of all Australians.
Using health-care workers’ full potential
The review involved extensive consultation, including on two issues papers. The report itself incorporates feedback from the consultations, including sceptical comments, reflecting a divergence of opinions.
Reflected the report’s title, Unleashing the Potential of our Health Workforce, its main emphasis is to change the rules and regulations imposed by state and federal governments. These stymie health professionals and limit their ability to use their full skills and knowledge to manage their patients’ care.
Over recent decades, health professionals’ education has improved. So professionals are capable of doing more than previously. Yet the rules and regulations have not advanced and so inhibit professionals from making those skills and knowledge available.
The review argues this contributes to career dissatisfaction, and to people leaving various health professions, exacerbating workforce shortages.
The review proposes a new way of documenting and describing what can be done by a profession through what it calls a National Skills and Capability Framework and Matrix.
As with many other recommendations, the review points to where this is done already internationally and how it can nestle into other policies and frameworks to aid implementation.
To the disappointment of most allied health professions, the review does not recommend more Medicare payments for them to practise independently.
Rather, the review recommends payment to general practices for them to expand multi-disciplinary teams. This would see professionals working together, rather than in competition or isolation.
The review also recommends changing the rules about referrals by health professionals, allowing qualified health professionals to refer directly to non-GP medical specialists in similar areas. This means your psychologist could refer you directly to a psychiatrist if needed, or your physiotherapist could refer you directly to an orthopaedic surgeon rather than needing to go back to your GP.
This will weaken the role of the GP as a “gatekeeper” and also potentially undermine the more holistic care that GPs provide. But from a patient’s point of view, eliminating the intermediate step saves them out-of-pocket costs.
An important recommendation recognises that the health system evolves and rules and regulations need to evolve too. It therefore supplements its recommendations for changes now, with an approach for continuous review through an independent mechanism. This would provide evidence-based advice and recommendations about:
- significant workforce innovation
- emerging health care roles
- workforce models that involve significant change to scope.
When will we see change?
The review sets out a loose timeline for implementation, described as short, medium and long term. And it assigns responsibility for each element of its recommendations to appropriate bodies and governments.
As almost all the recommendations require legislative change, and many require agreement between the Commonwealth and the states, it’s unlikely any of the changes will take effect this financial year.
The review recommends change be implemented in a systematic, evidence-based and safe way. Implementation would start in areas of greatest need such as in rural and remote Australia and also in practices most ready for the change, such as Aboriginal Controlled Community Health Organisations or Victoria’s Community Health Centres.
In releasing what he referred to as a “landmark” report, Health Minister Mark Butler noted the complexity of implementation, which would require collaborative action with states and territories. He noted the need for further consultation, but nevertheless took a supportive tone.
Can this review prompt real health reform?
Overall, the review charts a middle course between letting health professionals roam free and the tight and inappropriate rules and regulations which constrain patient care today. It also sets out the practical steps to achieve its goals.
The one downside of the report is the emphasis on harmonisation of state and territory approaches. This would replace the current approach, where each state and territory decides, for example, on what vaccines can be administered by which professionals and what pharmacists can dispense without a medical practitioner’s prescription.
One of the benefits of a federation is the potential for state- and territory-based innovation and cross-border learning. Harmonisation will limit that experimenting, and may lead to more of the stasis seen in health workforce policy in the past.
Authors: Stephen Duckett, Honorary Enterprise Professor, School of Population and Global Health, and Department of General Practice and Primary Care, The University of Melbourne